The Maryland Department of Health confirmed the first three cases of omicron Dec. If we knew in three weeks or six weeks in advance that we’re going to need more beds, you can more easily change around procedures and processes.” “We have these challenges that become acute when things rise dramatically, because it’s difficult to pivot quickly. 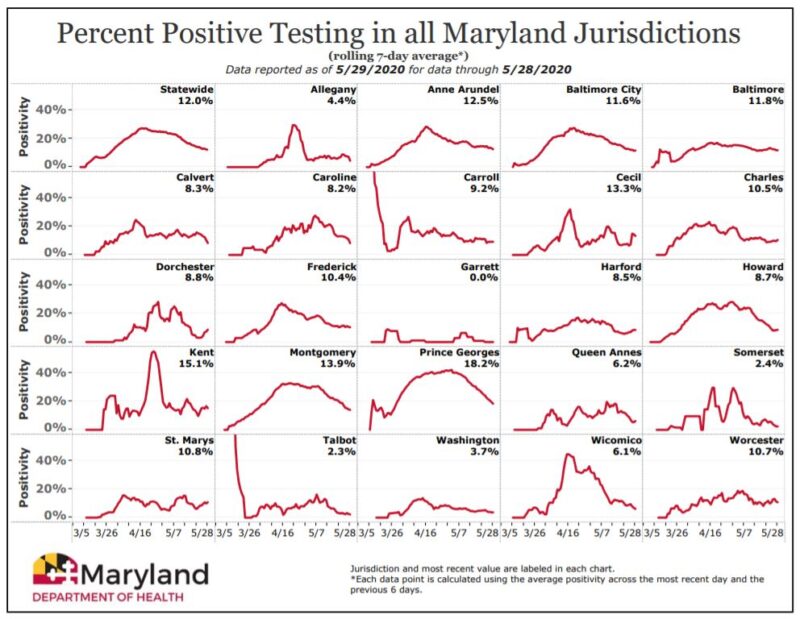
“We’re not clear on what’s happening now, so that’s the big question,” Klein said. Usually, more hospitalizations are caused by more cases, but with Maryland’s infection tally still unknown, the state’s models will not be complete. The change in weather, increase in indoor activities, and relaxation of mask mandates and social distancing requirements are more likely driving the uptick, he said. Omicron, he said, seems more transmissible but is probably not accounting for the current surge in hospitalizations. Under a worst-case scenario, cases could spike to levels not yet seen during the pandemic, or, with universal masking, they could plummet.Įili Klein, associate professor of emergency medicine at Johns Hopkins who researches how individuals contribute to the spread of infectious diseases, said the picture is less clear in Maryland where data gaps are clouding the view. Modeling from the University of Washington’s Institute for Health Metrics and Evaluation shows cases nationwide are expected to remain high through the end of January. Get vaccinated, get the booster, stay distant, wash your hands, and yes, wear a mask indoors and at gatherings.” Do the responsible thing to help us cope. 
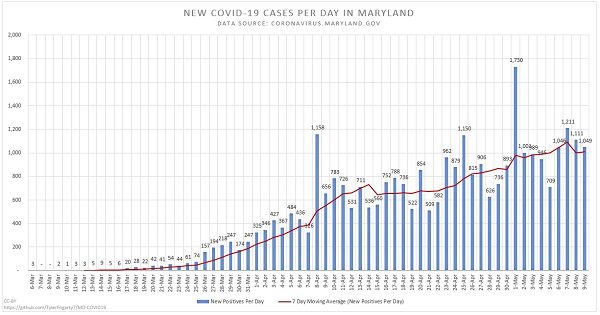
“People don’t want to wear masks anymore. “I get it, people want to celebrate the holidays with their families,” Simmons said. A bed or provider may not be readily available when people need them. She said the missing state data could help push that message by showing people just how bad things are getting and how fast.Įven without it, she said, hospitals already are overwhelmed and staffs are severely burned out. Simmons said the situation is so severe and the threats so strong that she called for reinstatement of a mask mandate, which Hogan and many other executives have resisted after public backlash. She recalled two unvaccinated patients - one 26, the other 52 - who had no underlying health conditions and recently died from the virus. Few are vaccinated and none have had booster shots now authorized for those 16 and older. She said many hospitalized patients are younger, ages 25 to 55. That is a crucial message, said Leslie Simmons, chief operating officer at LifeBridge Health, which operates Sinai hospital and others. Hogan also continued his calls for people to get vaccinated and boosted against COVID-19 and also against the flu, shots that can be given together. The number of COVID-19 cases has not been updated since Dec. 14, according to the state’s coronavirus dashboard. Hospitalizations were at 1,151 Tuesday, up from a recent low of 490 on Nov. Hogan specifically ordered hospitals to reduce non-urgent medical surgeries when hospitalizations reached 1,200 and implement their pandemic plans at 1,500. Larry Hogan made some of these actions official Wednesday as part of the state’s ongoing pandemic planning, and asked hospitals to submit specific surge plans in anticipation of more delta and omicron cases.įor its part, the state established a Surge Operation Center to manage, for example, patient transfers when hospitals are at capacity.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
